By Nancy Collins, PhD, RDN, LD, NWCC, FAND
We have made progress in reducing healthcare-associated infections, but still have a long way to go, especially when patients complain of dirty, dingy hospitals and clinics.
I feel a little like girl detective Nancy Drew as I ask you to consider the Case of the Dirty Wound Care Clinic. Let me explain. In a recent lawsuit, the plaintiff alleged that her mother’s wound did not heal and became infected because of the lack of cleanliness in the hospital-based clinic where she was receiving treatment. It would not surprise me if your initial reaction to this claim is that it is nonsense, so let’s take a closer look.
Healthcare-Associated Infection Rates
Hospitals serve vulnerable people, who often are carrying a plethora of germs. It is the perfect storm for infections, which is exactly why we have programs in place to address this situation. We have entire infection control teams devoted to education, training, and monitoring of these programs. With all this in place, it seems that this should control the problem. Some success has occurred, but the Centers for Disease Control and Prevention (CDC) says that on any given day, about 1 in 25 hospital patients has at least one healthcare-associated infection (HAI).
In 2014, results of a project known as the HAI Prevalence Survey were published. The survey described the burden of HAIs in US hospitals and reported that an estimated 722,000 HAIs occurred in US acute care hospitals in 2011. In addition, about 75,000 patients with HAIs died during their hospitalizations.1
Hospital Hygiene
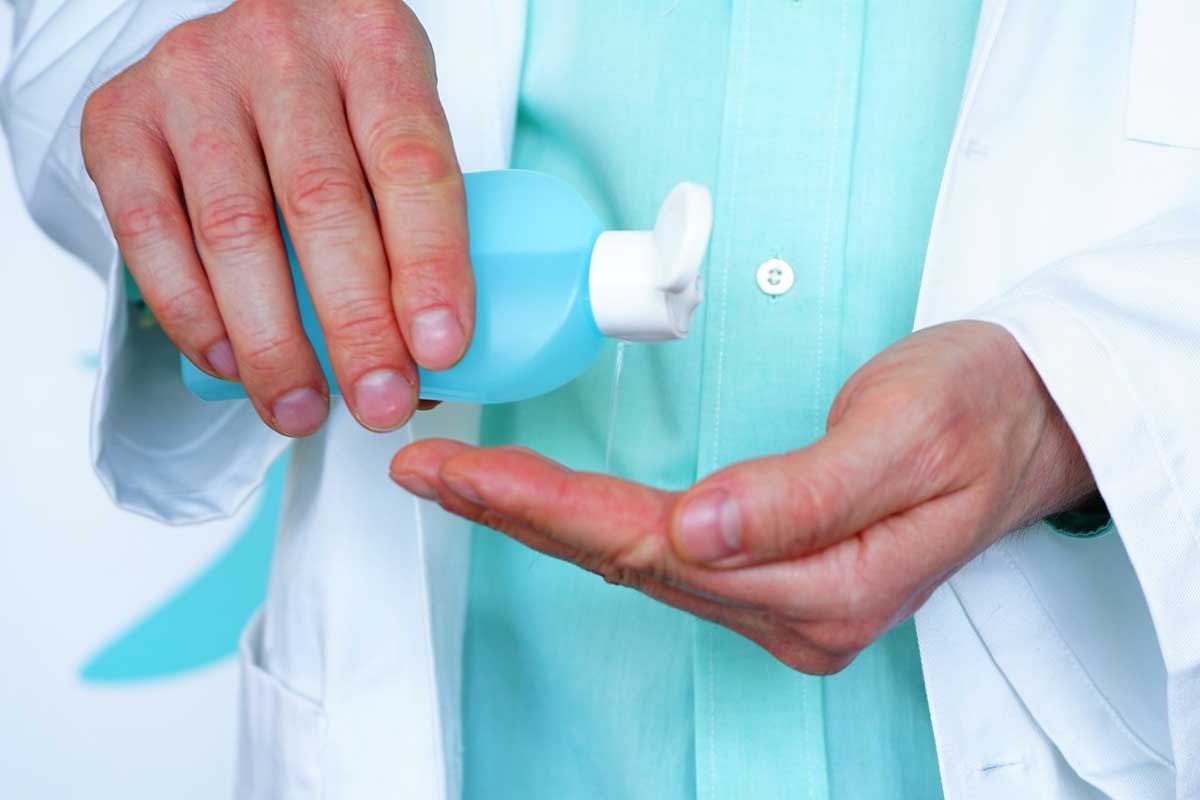
It seems that hand hygiene is accepted universally. We all know the importance of washing our hands. But what about lab coats, neckties, lanyards, cell phones, call buttons, and bedside tables? Would it trouble you to know that up to 70% of physicians admitted having never cleaned their ties?2 Lab coats are just as problematic.
A University of Maryland study showed that 65% of physicians and other medical professionals admitted they had not washed their lab coat in at least a week, even though they knew it was dirty. Nearly 16% said they had not put on a clean lab coat in at least a month.3 While this might not mean that these articles of clothing are infecting patients, it certainly does not help when a patient complains of a dirty facility.
Appearance Counts
The plaintiff in the lawsuit was asked to describe what troubled her about the wound clinic. She reported that it just seemed to have an unkempt appearance. She described peeling paint, scuffs on the doors and walls, a broken chair, and general clutter. She said the staff seemed overtaxed and was running late all the time, with wait times of over 1 hour beyond the appointment time. She recalled an instance when she had to prompt the nurse to change her gloves after dropping an item on the floor and picking it up with her gloved hand. These observations all seemed believable, and it appeared that the plaintiff was a caring and concerned daughter. In other words, she was a credible witness.
The defense witnesses countered that they operated one of the most respected wound care facilities in the state, staffed by highly qualified professionals. Yes, perhaps the physical plant was in need of some sprucing up and maybe some additional training was in order on infection control procedures. They maintained that there is a big jump from these admissions to concluding that the facility caused the patient’s wound infection. It seemed that the staff all were qualified professionals who genuinely cared for their patients. In other words, they were more good witnesses.
Solving the Case
We will never know exactly what caused this patient’s infection or why she suffered a rapid decline in condition. Yet, it is necessary to resolve the case somehow. Essentially there are two choices—make an out-of-court settlement or try the case in front of a jury. As in most of my cases, this one was settled with an out-of-court settlement. The facility and their insurance carrier felt it was less costly to offer a monetary settlement than risk a jury verdict.
While this is perhaps a less than palatable solution, it is often what happens. We have to try to improve and learn some lessons.
Some areas for possible improvement and thought:
- Infections are still a problem and need our attention. Make sure your policies and training are up to date.
- Conduct your own assessment. Kits are readily available to demonstrate if hand washing and surface cleaning techniques are adequate by lighting up germs with UV light. Check out http://www.glogerm.com/.4
- Appearances count. Make sure you and your clothing represent the professional status you carry.
- Physical plants need upkeep. Make sure to do repairs as needed and refreshes as budgets permit.
References
- Center for Disease Control and Prevention. HAI data and statistics. Centers for Disease Control and Prevention website. https://www.cdc.gov/HAI/surveillance/index.html.
- Bearman G, Bryant K, Leekha S, et al. Healthcare personnel attire in non-operating-room settings. Infect Control Hosp Epidemiol. 2014;35(2):107-121. doi:10.1086/675066.
- McCaughey B. Why aren’t hospitals cleaner? [commentary on Esterbrook J. US News & World Report. July 13, 2007]. CBS News website. https://www.cbsnews.com/news/why-arent-hospitals-cleaner/.
The original visual tool for teaching proper handwashing, aseptic techniques, and general infection control. Glo Germ website. http://www.glogerm.com/.